 Back
BackThe Reproductive System: Structure, Function, and Regulation
Study Guide - Smart Notes

Reproductive System Overview
Primary Sex Organs and Functions
The reproductive system consists of primary sex organs (gonads) and accessory reproductive organs. The gonads—testes in males and ovaries in females—produce gametes and secrete steroid sex hormones. Accessory organs include ducts, glands, and external genitalia, all of which support the transport and survival of gametes and facilitate fertilization.
Gonads: Testes (males), Ovaries (females)
Gametes: Sperm (males), Ova (females)
Hormones: Androgens (males), Estrogens and Progesterone (females)
Accessory Organs: Ducts, glands, external genitalia
Sex hormones regulate the development and function of reproductive organs, sexual behavior, and secondary sexual characteristics.
Male Reproductive System
Gross Anatomy of the Male Reproductive Tract
The male reproductive system is specialized for the production, maturation, and delivery of sperm. The testes are housed in the scrotum and connected to the exterior via a series of ducts and glands.
Testes: Produce sperm and testosterone
Scrotum: Sac that maintains testes at a temperature optimal for spermatogenesis
Duct System: Epididymis, ductus (vas) deferens, ejaculatory duct, urethra
Accessory Glands: Seminal vesicles, prostate, bulbourethral glands
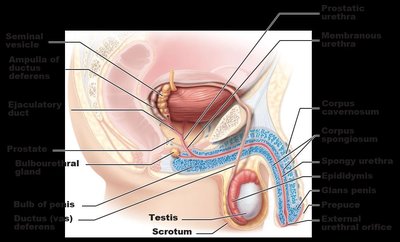
The Scrotum and Testes
The scrotum is a skin-covered sac that houses the testes outside the abdominopelvic cavity, maintaining a temperature about 3°C below core body temperature, which is essential for sperm production. Temperature is regulated by the dartos and cremaster muscles.
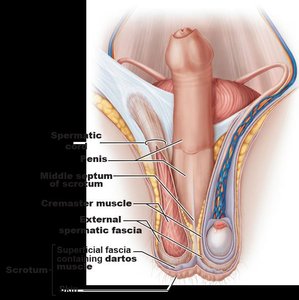
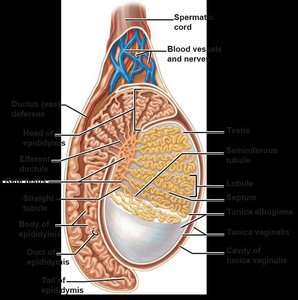
Internal Structure of the Testes
Each testis is surrounded by two tunics: the outer tunica vaginalis and the inner tunica albuginea. Septa divide the testis into lobules, each containing seminiferous tubules where spermatogenesis occurs. Interstitial (Leydig) cells between tubules produce androgens.
The Penis
The penis is composed of the root, shaft, and glans penis. It contains three cylindrical bodies of erectile tissue: two corpora cavernosa and one corpus spongiosum, which surrounds the urethra. Erection is achieved by engorgement of these tissues with blood.
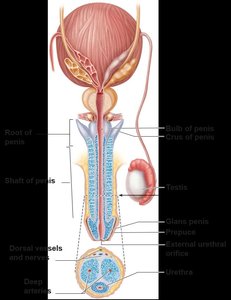
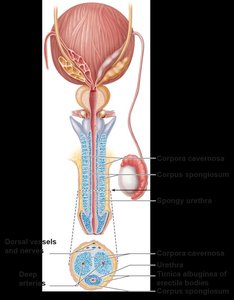
Male Duct System
Sperm travel from the testes through the epididymis (site of maturation), ductus deferens, ejaculatory duct, and urethra. The urethra serves both urinary and reproductive functions and is divided into prostatic, membranous, and spongy regions.
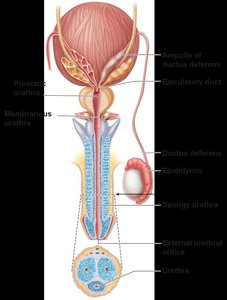
Accessory Glands and Semen
Accessory glands produce seminal fluid, which nourishes and protects sperm. The seminal vesicles contribute fructose and prostaglandins, the prostate adds enzymes and PSA, and the bulbourethral glands secrete mucus for lubrication and neutralization of acidic urine.
Semen: Mixture of sperm and glandular secretions; 2–5 mL per ejaculation, containing 20–150 million sperm/mL
Functions: Nutrient supply, pH buffering, motility enhancement, and antimicrobial activity
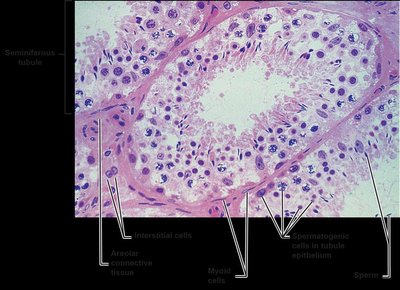
Spermatogenesis
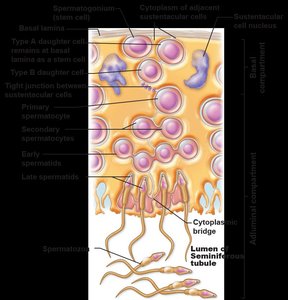
Spermatogenesis is the process by which sperm are produced in the seminiferous tubules. It involves mitosis, meiosis, and spermiogenesis (maturation of spermatids into spermatozoa).
Mitosis: Spermatogonia divide to produce primary spermatocytes
Meiosis: Primary spermatocytes undergo two meiotic divisions to form spermatids
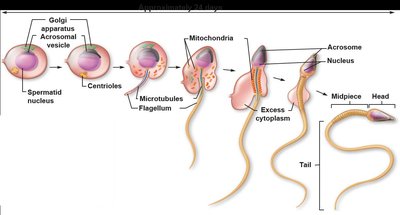
Spermiogenesis: Spermatids mature into spermatozoa
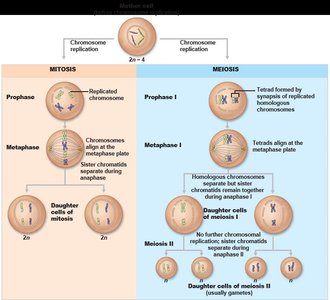
Hormonal Regulation of Male Reproductive Function
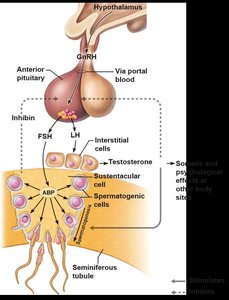
The hypothalamic-pituitary-gonadal (HPG) axis regulates spermatogenesis and testosterone production. GnRH from the hypothalamus stimulates FSH and LH release from the anterior pituitary. FSH acts on sustentacular (Sertoli) cells, while LH stimulates Leydig cells to produce testosterone. Negative feedback is provided by rising testosterone and inhibin levels.
Male Secondary Sex Characteristics and Sexual Response
Testosterone induces secondary sex characteristics such as increased muscle mass, deepening of the voice, and growth of body hair. Male sexual response involves erection (parasympathetic) and ejaculation (sympathetic).
Female Reproductive System
Gross Anatomy of the Female Reproductive Tract
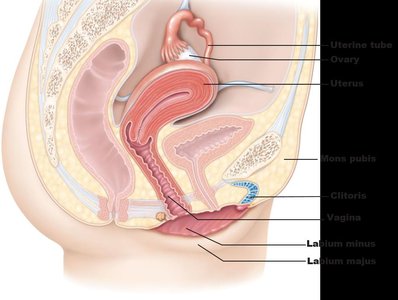
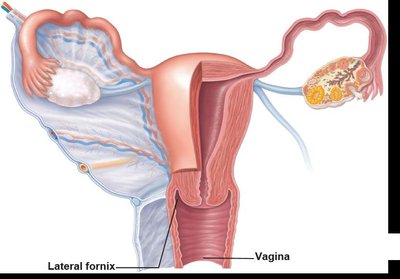
The female reproductive system includes the ovaries, uterine tubes, uterus, vagina, and external genitalia (vulva). The ovaries produce ova and secrete estrogen and progesterone.
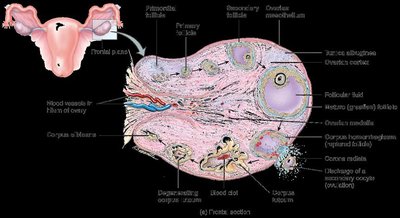
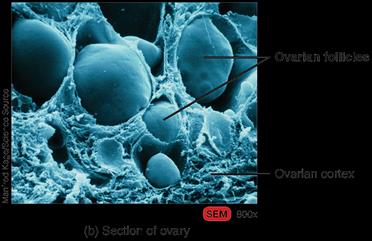
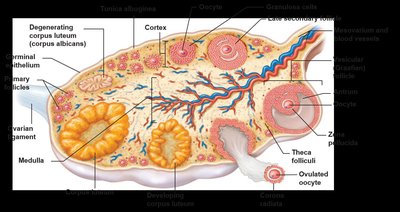
Ovarian Structure and Follicle Development
The ovary is divided into a cortex (containing follicles) and medulla (containing blood vessels and nerves). Follicles develop through several stages: primordial, primary, secondary, late secondary, and vesicular (Graafian) follicle. Ovulation releases a secondary oocyte, and the ruptured follicle becomes the corpus luteum.
Female Duct System
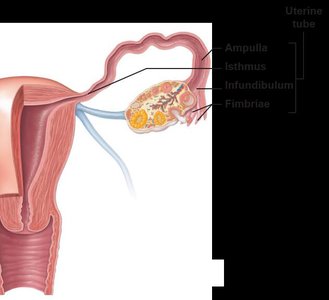
The uterine (fallopian) tubes transport the oocyte from the ovary to the uterus. Fertilization usually occurs in the ampulla. The uterus is a muscular organ with three layers: perimetrium, myometrium, and endometrium. The endometrium undergoes cyclic changes during the menstrual cycle.
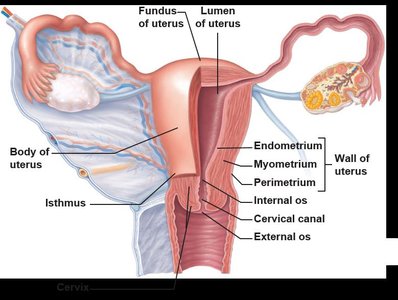
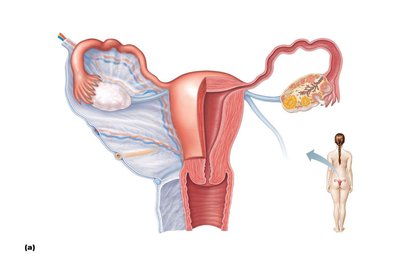
Uterine Wall and Blood Supply
The endometrium consists of the stratum functionalis (shed during menstruation) and stratum basalis (regenerates new functionalis). The uterine arteries branch into arcuate and radial arteries, with spiral arteries supplying the functionalis and straight arteries supplying the basalis.
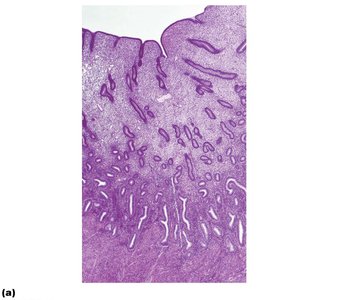
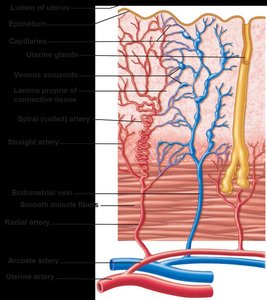
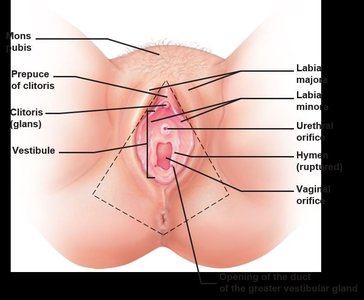
Vagina and External Genitalia
The vagina serves as the birth canal and organ of copulation. The external genitalia (vulva) include the mons pubis, labia majora and minora, clitoris, and vestibule. Greater vestibular glands secrete mucus for lubrication.
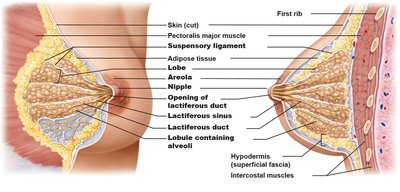
Mammary Glands
Mammary glands are modified sweat glands that produce milk. Each breast contains 15–25 lobes with lobules containing alveoli. Milk is conveyed through lactiferous ducts and sinuses to the nipple.

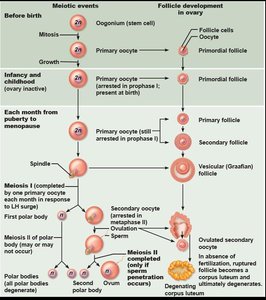
Oogenesis
Oogenesis is the process of ovum formation. It begins in the fetal period, with oogonia dividing by mitosis and forming primary oocytes that arrest in prophase I. Each month after puberty, a few primary oocytes resume meiosis, producing a secondary oocyte (arrested in metaphase II) and a polar body. If fertilization occurs, meiosis II completes, yielding an ovum and a second polar body.
Ovarian Cycle
The ovarian cycle consists of the follicular phase (days 1–14, follicle growth), ovulation (midcycle), and luteal phase (days 14–28, corpus luteum activity). Hormonal regulation involves GnRH, FSH, LH, estrogen, progesterone, and inhibin.
Hormonal Interactions During the Ovarian Cycle
GnRH stimulates FSH and LH release, promoting follicle growth and estrogen production. High estrogen levels trigger an LH surge, causing ovulation and corpus luteum formation. The corpus luteum secretes progesterone, estrogen, and inhibin, which inhibit FSH and LH. If no pregnancy occurs, hormone levels fall, and the cycle restarts.
Uterine (Menstrual) Cycle
The uterine cycle describes cyclic changes in the endometrium in response to ovarian hormones. It consists of three phases:
Menstrual phase (days 1–5): Shedding of the stratum functionalis
Proliferative phase (days 6–14): Regeneration of the functionalis under estrogen influence
Secretory phase (days 15–28): Endometrial preparation for implantation under progesterone influence
Effects of Estrogens and Progesterone
Estrogens promote oogenesis, follicle growth, and secondary sex characteristics. Progesterone works with estrogen to regulate the uterine cycle and supports pregnancy by inhibiting uterine motility and preparing the breasts for lactation.
Female Sexual Response
Female sexual response is initiated by touch and psychological stimuli, leading to engorgement of the clitoris, vaginal mucosa, and breasts. Lubrication is provided by vestibular gland secretions. Orgasm involves muscle tension, increased pulse and blood pressure, and uterine contractions.
Birth Control and Abortion
Birth Control Methods
Birth control methods prevent conception and include abstinence, surgical sterilization, hormonal methods, and periodic abstinence. Complete abstinence is the only 100% effective method.
Abortion
Abortion is the premature expulsion of the products of conception. Methods include pharmacological (e.g., mifepristone), vacuum aspiration, dilation and evacuation, and late-stage procedures.
Aging and Homeostatic Imbalances of the Reproductive System
Aging
Reproductive function declines with age. In women, ovarian follicles are depleted by age 30–40, leading to decreased estrogen. In men, testosterone and sperm levels decline after age 55, and benign prostatic hypertrophy is common after age 60.
Homeostatic Imbalances
Men: Testicular cancer, prostate disorders, erectile dysfunction
Women: PMS, premenstrual dysphoric disorder, endometriosis, breast and ovarian cancer, yeast infection
Both: Sexually transmitted diseases (chlamydia, trichomoniasis, gonorrhea, syphilis, genital herpes, genital warts)
