 Back
BackThe Urinary System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Urinary System
Introduction to the Urinary System
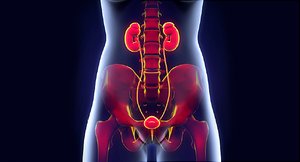
The urinary system is essential for filtering blood, removing waste, and maintaining homeostasis. It consists of the kidneys, ureters, urinary bladder, and urethra, each with specialized roles in urine formation and excretion.
Kidneys: Filter blood, remove waste, and convert filtrate into urine.
Ureters: Muscular tubes that transport urine from the kidneys to the urinary bladder.
Urinary Bladder: Expandable muscular sac that stores urine (up to 1 L).
Urethra: Tube that eliminates urine from the body.
Other Functions of the Kidneys
Regulation of Ion Levels and Acid-Base Balance: Controls blood concentrations of ions such as Na+, K+, and Ca2+; maintains acid-base balance by altering H+ and HCO3- levels.
Production and Release of Erythropoietin (EPO): In response to low blood oxygen, kidneys secrete EPO, stimulating red bone marrow to increase erythrocyte production.
Regulation of Blood Pressure: Alters urine output to regulate blood volume and releases renin, which is required for the production of angiotensin II, a hormone that increases blood pressure.
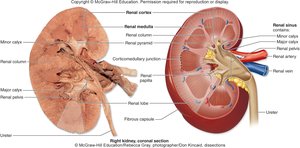
Gross Anatomy of the Kidney
Kidney Characteristics
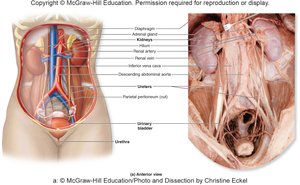
The kidneys are paired, bean-shaped organs located retroperitoneally. Each has a concave medial border (hilum) for entry/exit of vessels, nerves, and the ureter. The adrenal gland sits atop each kidney.
Functional Anatomy of the Kidney
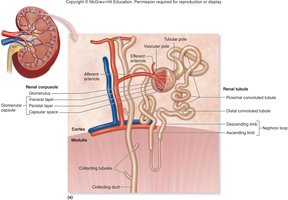
Nephron Structure
The nephron is the microscopic functional unit of the kidney, responsible for filtration and urine formation. Each nephron consists of a renal corpuscle and a renal tubule, mostly located in the cortex.
Renal Corpuscle: Includes the glomerulus and Bowman's capsule.
Renal Tubule: Composed of the proximal convoluted tubule (PCT), nephron loop (loop of Henle), and distal convoluted tubule (DCT).
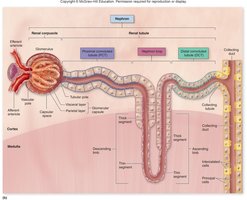
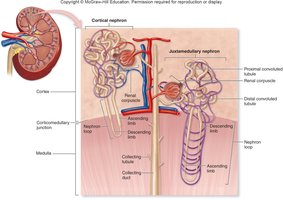
Types of Nephrons
Cortical Nephrons: Located primarily in the cortex; make up about 85% of nephrons.
Juxtamedullary Nephrons: Located near the corticomedullary junction; have long nephron loops that extend deep into the medulla, crucial for concentrating urine.
Collecting Tubules and Collecting Ducts
Nephrons drain into collecting tubules, which then empty into larger collecting ducts. These structures project toward the renal papilla, where fluid empties into a papillary duct.
Juxtaglomerular Apparatus (JG Apparatus)
The JG apparatus regulates blood filtrate formation and systemic blood pressure. It consists of granular cells (modified smooth muscle cells that secrete renin) and macula densa cells (epithelial cells that sense NaCl concentration in the DCT and signal granular cells).
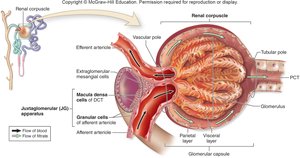
Blood Flow and Filtrate Flow in the Kidney
Blood Supply to the Kidneys
About 20–25% of resting cardiac output flows through the kidneys. Filtrate forms as blood passes through the glomerulus, with some plasma components entering the capsular space.
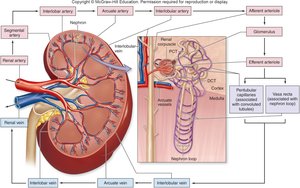
Filtrate, Tubular Fluid, and Urine Flow
Filtrate is formed when water and solutes are filtered from blood plasma across the glomerular capillaries into the capsular space. This filtrate then passes through the nephron and collecting system, undergoing modification to become urine.
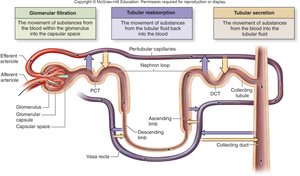
Overview of Urine Formation Processes
Glomerular Filtration: Movement of substances from blood into the capsular space.
Tubular Reabsorption: Movement of substances from tubular fluid back into the blood.
Tubular Secretion: Movement of substances from blood into the tubular fluid.
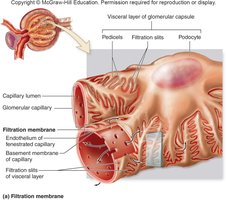
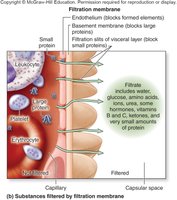
Filtration Membrane
The filtration membrane consists of three layers: the endothelium of glomerular capillaries, the basement membrane, and the filtration slits of podocytes. It allows passage of water and small solutes but restricts large proteins and cells.
Glomerular Filtration and Its Regulation
Pressures Associated with Glomerular Filtration
Net filtration pressure (NFP) is determined by the balance of hydrostatic and osmotic pressures:
Hydrostatic Pressure (HPg): Blood pressure in the glomerulus (e.g., 60 mm Hg).
Osmotic Pressure (OPg): Due to plasma proteins (e.g., 32 mm Hg).
Capsular Hydrostatic Pressure (HPc): Pressure in the capsular space (e.g., 18 mm Hg).
The equation for NFP is:
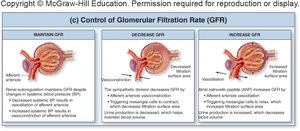
Regulation of Glomerular Filtration Rate (GFR)
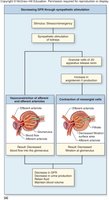
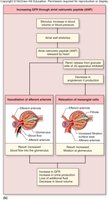
GFR is the volume of fluid filtered per minute. It is tightly regulated by intrinsic (renal autoregulation) and extrinsic (neural and hormonal) mechanisms to maintain homeostasis.
Intrinsic Controls: Myogenic response and tubuloglomerular feedback maintain constant GFR despite changes in systemic blood pressure.
Extrinsic Controls: Sympathetic stimulation decreases GFR; atrial natriuretic peptide (ANP) increases GFR.
Reabsorption and Secretion in the Nephron
Complete Reabsorption of Substances
Nutrients: Glucose and amino acids are normally 100% reabsorbed in the PCT via specific transport proteins.
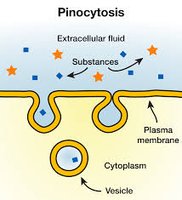
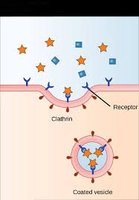
Filtered Plasma Proteins: Most proteins are not filtered, but small amounts are reabsorbed by pinocytosis or receptor-mediated endocytosis.
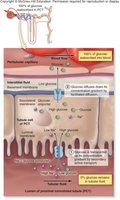
Sodium Reabsorption
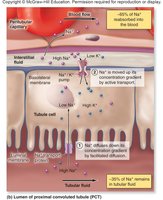
Sodium reabsorption is driven by Na+/K+ pumps in the basolateral membrane, requiring energy. It is regulated by hormones such as aldosterone (increases reabsorption) and ANP (decreases reabsorption).
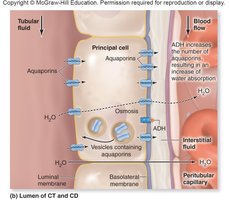
Water Reabsorption
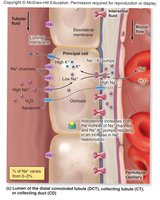
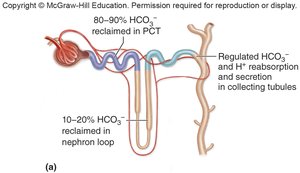
Most water is reabsorbed in the PCT (65%) via aquaporins. In the nephron loop, 10% is reabsorbed. In the DCT and collecting ducts, water reabsorption is regulated by aldosterone and antidiuretic hormone (ADH), which increase the number of aquaporins and thus water reabsorption.
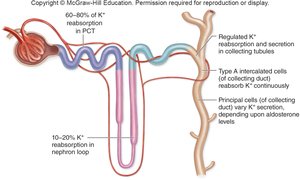
Potassium, Calcium, and Phosphate Balance
Potassium: Reabsorbed and secreted depending on aldosterone and the needs of the body.
Calcium and Phosphate: Parathyroid hormone (PTH) increases Ca2+ reabsorption in the DCT and inhibits PO43- reabsorption in the PCT.
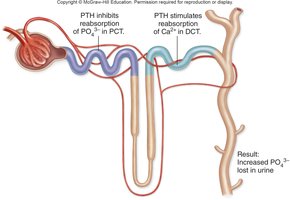
Bicarbonate Ions, Hydrogen Ions, and pH Regulation
The kidneys regulate blood and urine pH by reabsorbing or secreting HCO3- and H+ in the collecting tubules. Type A intercalated cells secrete H+ and reabsorb HCO3- (acidic blood), while Type B cells do the opposite (alkaline blood).
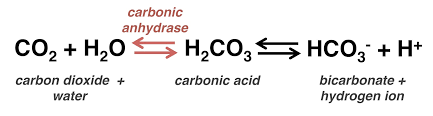
Substances Eliminated as Waste Products
Metabolic Wastes: Urea (from protein breakdown), uric acid (from nucleic acid breakdown), and creatinine (from muscle metabolism) are eliminated in urine.
Other Substances: Hormones, metabolites, and foreign substances are also excreted.
Establishing the Concentration Gradient
The interstitial fluid surrounding the nephron and collecting duct has a concentration gradient, established by solutes such as Na+ and Cl-, which increases from cortex to medulla. This gradient is essential for water reabsorption, especially under the influence of ADH.
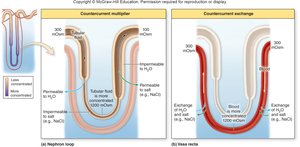
Urea Recycling
Urea is recycled between the collecting duct and nephron loop, contributing to the concentration gradient in the medulla and aiding in water reabsorption.



Renal Function and Urine Characteristics
Measuring Renal Plasma Clearance
Renal plasma clearance tests assess kidney function by measuring the volume of plasma cleared of a substance per minute. Substances can be filtered, reabsorbed, or secreted, affecting their clearance rates (e.g., inulin, glucose, creatinine).
Characteristics of Urine
Composition: Water, urea, ions, and other waste products.
Volume: Varies with hydration status.
Specific Gravity: Normal range is 1.005 to 1.030.
pH, Color, Turbidity, Smell: Diagnostic indicators; urinalysis is a common test.
Urinary Tract: Ureters, Bladder, and Urethra
Ureters
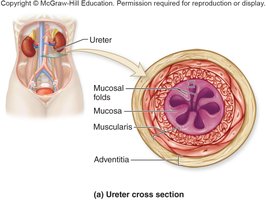
Ureters are long, epithelial-lined fibromuscular tubes that conduct urine from the kidneys to the urinary bladder. Their walls consist of three tunics: mucosa, muscularis, and adventitia.
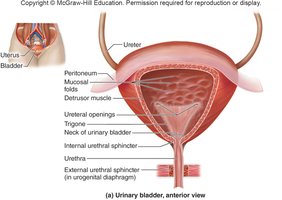
Urinary Bladder
The urinary bladder is a muscular sac with mucosa, submucosa, muscularis, and adventitia layers. It stores urine until micturition.
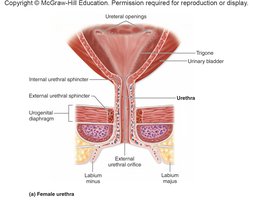
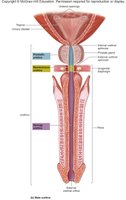
Urethra
The urethra is the terminal tube for urine excretion. Its structure differs between females and males.
Female Urethra: Shorter, opens anterior to the vaginal opening.
Male Urethra: Longer, passes through the penis and serves both urinary and reproductive functions.
Micturition (Urination)
Reflexes and Control
Storage Reflex: Sympathetic stimulation relaxes the detrusor muscle and contracts the internal urethral sphincter, retaining urine. The external urethral sphincter is kept contracted by the pudendal nerve.
Micturition Reflex: When bladder volume reaches 200–300 mL, stretch receptors activate the micturition center in the pons, increasing parasympathetic signals that contract the detrusor muscle and relax the internal sphincter.
Conscious Control: The cerebral cortex can voluntarily relax the external urethral sphincter, allowing urination. The Valsalva maneuver (abdominal muscle contraction) can facilitate urination.
