 Back
BackCardiovascular Disease: Epidemiology, Risk Factors, Pathology, and Prevention
Study Guide - Smart Notes

Cardiovascular Disease: Overview
Definition and Types
Cardiovascular disease (CVD) refers to a group of disorders affecting the heart and blood vessels. It is the leading cause of death globally and encompasses several conditions:
Coronary heart disease: Disease of the blood vessels supplying the heart muscle.
Cerebrovascular disease: Disease of the blood vessels supplying the brain.
Peripheral arterial disease: Disease of blood vessels supplying the arms and legs.
Rheumatic heart disease: Damage to the heart muscle and valves from rheumatic fever.
Congenital heart disease: Malformations of heart structure present at birth.
Deep vein thrombosis and pulmonary embolism: Blood clots in the leg veins that can travel to the heart and lungs.

Epidemiology
Epidemiology studies the distribution and determinants of health problems in populations.
CVDs are responsible for approximately 32% of all global deaths (19.8 million in 2022).
85% of CVD deaths are due to heart attack and stroke.
Over three-quarters of CVD deaths occur in low- and middle-income countries.
Coronary heart disease is the most common type in the USA, causing over 370,000 deaths in 2022.

Coronary Artery Disease (CAD)
Definitions and Clinical Spectrum
Coronary artery disease (CAD) is characterized by atherosclerosis in the coronary arteries, which may be asymptomatic.
Coronary heart disease (CHD) or ischemic heart disease (IHD) includes stable angina, acute coronary syndrome (ACS), and silent myocardial ischemia.
Acute coronary syndrome (ACS) includes unstable angina and myocardial infarction, typically symptomatic.
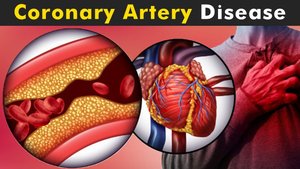
Risk Factors for Cardiovascular Disease
Modifiable Risk Factors
Modifiable risk factors are those that can be changed to reduce disease risk:
Hypertension (high blood pressure)
Raised cholesterol (especially LDL)
Metabolic disease (e.g., diabetes)
Obesity (especially increased waist circumference)
Smoking
Unhealthy diet (high in saturated fats)
Physical inactivity
Excessive alcohol use
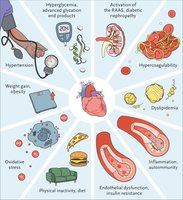
Non-Modifiable Risk Factors
Age
Gender
Ethnicity
Family history of early heart attack or raised cholesterol
Population Disparities
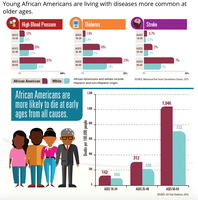
CVD age-adjusted death rates are 33% higher for Black Americans than the overall U.S. population.
Black Americans are nearly twice as likely to have a first stroke and more likely to die from one than White Americans.
Native Americans and Alaskans have higher early death rates from heart disease.
Etiology of Cardiovascular Disease
Intrinsic and Extrinsic Causes
Intrinsic (internal): Genetic, psychological factors
Extrinsic (external): Infectious diseases, environmental exposures

Etiology of Coronary Artery Disease
Smoking is the most significant risk factor.
High LDL cholesterol increases risk.
Chronic inflammation, obesity, and metabolic disease are important contributors.
Waist circumference is a better indicator of risk than BMI alone.

Pathophysiology of Atherosclerosis
Plaque Formation
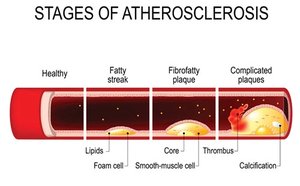
Plaque is a buildup of fatty material that narrows arteries and impedes blood flow.
Initial step: Formation of a "fatty streak" by subendothelial deposition of lipid-laden macrophages (foam cells).
Progression: Inflammatory cells and smooth muscle cells contribute to plaque growth and stability.
Stable plaques have thick fibrous caps; unstable plaques have thin caps and are prone to rupture, leading to heart attack or stroke.
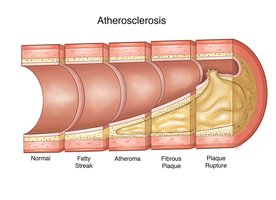
Clinical Manifestations
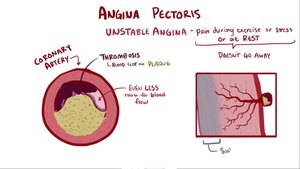
Angina
Gradual onset of chest discomfort, often triggered by exertion or stress.
Pain may radiate to the left arm, neck, jaw, or back.
Stable angina occurs with exertion and resolves with rest; unstable angina can occur at rest and has a worse prognosis.
Blood Pressure and Cardiovascular Disease
Blood Pressure Basics
Measured as systolic (maximum during contraction) over diastolic (minimum during relaxation) pressure in mm Hg.
Hypertension is defined as systolic ≥130 mm Hg or diastolic ≥80 mm Hg.
Primary hypertension has no known cause; secondary hypertension is due to identifiable conditions (e.g., kidney disease).
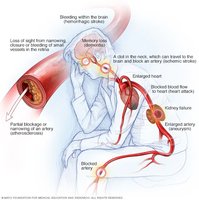
Consequences of High Blood Pressure
Damaged and narrowed arteries
Aneurysm formation
Heart failure and left ventricular enlargement
Stroke, dementia, and kidney damage
Cholesterol and Lipoproteins
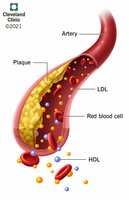
Role of Cholesterol
Essential for cell membrane structure, hormone synthesis, and vitamin D production.
Transported in blood as part of lipoproteins (HDL, LDL, VLDL, etc.).
High LDL is associated with increased risk of atherosclerosis; HDL is protective.
Prevention of Cardiovascular Disease
Levels of Prevention
Primary prevention: Prevent disease before it occurs (e.g., healthy diet, exercise, vaccinations).
Secondary prevention: Detect and treat early disease (e.g., screening, statins for high cholesterol).
Tertiary prevention: Reduce complications in established disease (e.g., rehabilitation after stroke).


Models of Health
Biomedical Model
Assumes all illness has a single underlying cause (disease/pathology).
Removal of disease restores health.
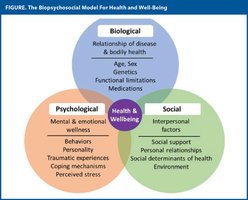
Biopsychosocial Model
Considers biological, psychological, and social factors in health and disease.
Recognizes the importance of mental health, social support, and environment.
Social Determinants, Health Equity, and Disparities
Determinants of Health
Genetics, behavior, environment, medical care, and social factors all influence health outcomes.
Health Equity
Achieved when everyone has the opportunity to be as healthy as possible.
Requires addressing social, economic, and environmental disparities.

Health Disparities
Preventable differences in health outcomes among socially disadvantaged groups.
Linked to race, ethnicity, socioeconomic status, and access to care.

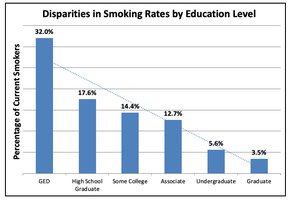
Socioeconomic Status and Health
Lower socioeconomic status is associated with poorer health outcomes.
Education, income, and occupation are key measures.
Racism and Health
Racism creates social and environmental conditions that disadvantage people of color, increasing risk for poor health outcomes.
Barriers include access to care, education, employment, and safe environments.
Evidence-Based Medicine and Prevention Strategies
Evidence-Based Medicine (EBM)
Combines best available research, clinical expertise, and patient values for optimal care.
Steps: Define question, search evidence, appraise, apply, and evaluate.
Prevention Strategies
Population-wide approaches: Reduce tobacco use, unhealthy diet, obesity, physical inactivity, and harmful alcohol use.

