 Back
BackPrimary Health Care and Healthy Public Policy: Foundations for Personal Health
Study Guide - Smart Notes

Primary Health Care (PHC): Foundations and Principles
Definition and Scope of PHC
Primary Health Care (PHC) is a comprehensive, principle-based approach to health service delivery that spans the entire continuum of care, from birth to death, and across all settings. PHC places individuals and communities at the center of care, aiming to improve the health of all people by addressing their needs holistically and equitably.
Comprehensive Care: Includes health promotion, disease prevention, treatment, emergency services, mental health care, palliative care, maternal and child health, rehabilitation, and specialist referrals.
Interprofessional Teams: Care is provided by teams of professionals who coordinate services to ensure continuity and quality.
Population Health: PHC is a key method for delivering public health and health promotion, focusing on the health of populations rather than just individuals.

Primary Care vs. Primary Health Care
Primary care is a component of PHC, focusing on community-based clinical services such as prevention, diagnosis, treatment, and management of health conditions. PHC, however, encompasses a broader approach, integrating social determinants and health promotion.
Primary Care: Direct clinical services, coordination of care, and access to other health services.
PHC: Broader focus including social, economic, and environmental factors affecting health.
Principles of Primary Health Care
The principles of PHC guide its implementation and ensure equitable, effective health services for all.
Accessibility: Health services must be available to all, regardless of ability to pay or location.
Active Public Participation: Communities are involved in planning and delivering services, fostering empowerment and ownership.
Health Promotion and Chronic Disease Prevention: Emphasizes prevention and upstream approaches rather than solely curative care.
Technology and Innovation: Use of appropriate, sustainable technology that is effective and acceptable to both providers and the public.
Intersectoral Cooperation: Collaboration across sectors such as education, environment, and justice to address the broad determinants of health.

Health Promotion and Healthy Public Policy
Health Promotion (HP)
Health promotion is the process of enabling people to increase control over and improve their health. It involves building healthy public policy, creating supportive environments, strengthening community action, developing personal skills, and reorienting health services.
Empowerment: Helping individuals and communities gain control over health determinants.
Ottawa Charter (1986): Framework for health promotion emphasizing policy, environment, and community action.
Healthy Public Policy
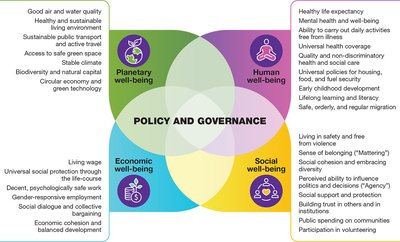
Healthy public policy refers to government decisions that deliberately aim to improve the health and welfare of populations. Such policies prioritize health and equity in all areas and hold policymakers accountable for health outcomes.
Social Justice and Equity: Policies should address root causes of ill-health and promote fairness.
Community Participation: Engaging communities in decision-making ensures policies are relevant and sustainable.
Challenges in Health Promotion and PHC
Barriers to Health Promotion
Despite its importance, health promotion faces several challenges:
Lack of Understanding: Policymakers may not fully grasp health promotion concepts.
Education Gaps: Many professionals are not trained in community development or health promotion strategies.
Systemic Focus on Disease: Traditional health systems prioritize treatment over prevention.
Evaluation Difficulties: Measuring health promotion outcomes and needs can be complex.
Resource Constraints: Limited funding and short-term political mandates hinder long-term progress.
Barriers to PHC Implementation
Expert vs. Client-Driven Services: Balancing professional expertise with community input can be challenging.
Interdisciplinary Collaboration: Overcoming silo mentalities and territoriality among disciplines and departments.
Resource Limitations: Financial and human resources are often insufficient.
Measuring Success: Health outcomes may take years to manifest, complicating evaluation.
Role of Nurses in PHC
Nurses as Key PHC Providers
Registered Nurses (RNs), Community Health Nurses, and Nurse Practitioners play a central role in PHC due to their holistic practice and broad knowledge base. They are equipped to address the diverse needs of individuals and communities, advocate for health equity, and implement health promotion strategies.

Social Marketing in Health Promotion
Definition and Purpose
Social marketing applies commercial marketing principles to design and implement programs that promote socially beneficial behaviors. The goal is to influence voluntary behavior change for improved personal and societal health.
Key Elements: Analysis, planning, execution, and evaluation of campaigns targeting specific audiences.
Examples: Public health campaigns like "Just do it!" or "Eat Fresh" use branding and messaging to encourage healthy choices.
Social Marketing Strategies
Social Modeling: Using influential figures or relatable scenarios to demonstrate desired behaviors.
Imagery and Branding: Creating memorable visuals and slogans to reinforce messages.
Competition: Addressing competing messages or behaviors in the environment.
The 5 P’s of Social Marketing
P | Description |
|---|---|
Product | The desired social action and its benefits |
Price | Costs (financial, emotional, time, effort) associated with the behavior |
Place | Where the behavior is performed and how it is made accessible |
Promotion | Methods and channels used to reach the audience |
Policy | Rules or regulations that support behavior change |

Ethical Principles in Health Promotion
Guiding Ethics for Health Professionals
Ethical principles provide a foundation for professional conduct in health promotion, guiding relationships, behaviors, and decision-making. They ensure care is delivered safely, compassionately, and equitably, and that barriers to care are addressed.
Autonomy/Self-Determination: Respecting individuals' rights to make informed choices about their health.
Informed Consent: Ensuring individuals understand and agree to interventions.
Confidentiality: Protecting personal health information.
Veracity: Commitment to truthfulness and transparency.
Nonmaleficence: Obligation to do no harm.
Beneficence: Promoting the well-being of individuals and communities.
Justice: Ensuring fairness and equity in health care delivery.

Additional info: These principles are further detailed in the Canadian Nurses Association Code of Ethics and are essential for advocacy and quality practice environments.
