 Back
BackPsychological Disorders II: Anxiety, OCD, Mood Disorders, and Schizophrenia
Study Guide - Smart Notes

Anxiety, Obsessive-Compulsive, & Depressive Disorders
Anxiety Disorders
Anxiety disorders are characterized by excessive, irrational, and maladaptive fear or nervousness. These disorders are common and often comorbid with other psychological conditions. Symptoms can include physiological responses such as fight-or-flight, freeze, or faint reactions. Anxiety disorders can significantly impair daily functioning and are not a sign of mental weakness.
Generalized Anxiety Disorder (GAD): Marked by frequently elevated levels of anxiety, often in response to everyday life challenges. Individuals experience a general sense of unease that is difficult to control, often linked to heightened amygdala sensitivity to stressors.
Panic Disorder: Characterized by sudden, intense episodes of fear known as panic attacks. Individuals may develop agoraphobia, a fear of having a panic attack in public places.
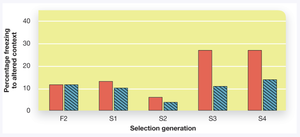
Specific Phobia: Involves intense fear of a particular object, activity, or organism. Genetic factors may contribute, as seen in selective breeding studies of fear responses.
Social Phobia (Social Anxiety Disorder): Involves a strong fear of being judged or embarrassed in social situations. Cultural variants such as hikikomori (extreme social withdrawal) are also observed.

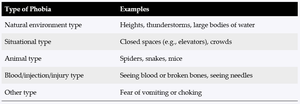
Type of Phobia | Examples |
|---|---|
Natural environment type | Heights, thunderstorms, large bodies of water |
Situational type | Closed spaces (e.g., elevators), crowds |
Animal type | Spiders, snakes, mice |
Blood/injection/injury type | Seeing blood or broken bones, seeing needles |
Other type | Fear of vomiting or choking |

Example: A student with social anxiety may arrive early to class to avoid crowded seating, buy food to go to avoid cafeterias, or pretend to use their phone to avoid social interaction.
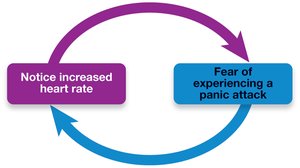
Panic Attack Cycle: Individuals may notice an increased heart rate, which leads to fear of experiencing a panic attack, further increasing anxiety.
Obsessive-Compulsive Disorder (OCD)
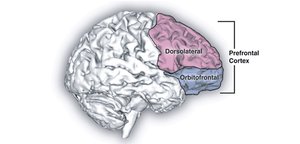
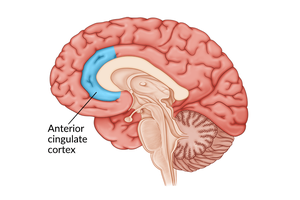
OCD is characterized by persistent, unwanted thoughts (obsessions) and repetitive, ritualistic behaviors (compulsions) performed to reduce anxiety. Common obsessions include fears of contamination, while compulsions may involve excessive cleaning or checking. The disorder is associated with dysfunction in the orbitofrontal cortex (OFC), basal ganglia, and thalamus, as well as the dorsolateral prefrontal cortex (DLPFC) and anterior cingulate cortex (ACC).
Obsessions: Intrusive thoughts that cause distress (e.g., fear of germs).
Compulsions: Ritualistic behaviors aimed at reducing anxiety (e.g., handwashing).
Neural Circuitry: The orbitofrontal loop (OFC → basal ganglia → thalamus) is implicated, along with the DLPFC and ACC.
Example: The "Lady Macbeth effect" refers to the urge to cleanse oneself after moral transgressions, illustrating the link between obsessions and compulsions.
Mood Disorders
Major Depressive Disorder (MDD)
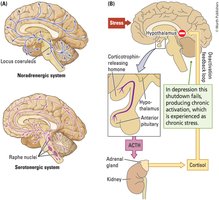
MDD involves prolonged periods of sadness, feelings of worthlessness, hopelessness, social withdrawal, and cognitive and physical sluggishness. Individuals may exhibit a pessimistic explanatory style, attributing negative events to internal, stable, and global causes. Neurobiological factors include amygdala hyperactivity, dysregulation of the HPA axis, reduced neurogenesis in the hippocampus, and altered function in the nucleus accumbens and medial prefrontal cortex (mPFC).
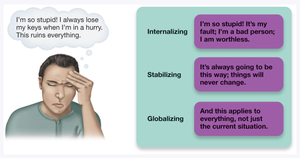
Pessimistic Explanatory Style: Internalizing (blaming oneself), stabilizing (believing things will never change), and globalizing (applying negativity to all situations).
Neurobiology: Overactivity of the amygdala, impaired inhibition by the hippocampus and frontal cortex, and reduced neurogenesis in the hippocampus.
Anhedonia: Loss of pleasure, linked to the nucleus accumbens.
Rumination: Persistent focus on negative thoughts, associated with the mPFC.
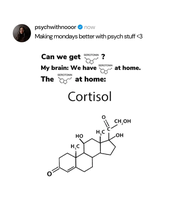
Serotonin (5-HT) and SSRIs: Serotonin dysregulation is implicated; selective serotonin reuptake inhibitors (SSRIs) are commonly prescribed.
Bipolar Disorder: Characterized by extreme mood swings from mania (elevated mood, energy, and activity) to depression. Bipolar disorder is difficult to treat and involves complex neurobiological mechanisms.
Schizophrenia
Symptoms and Phases
Schizophrenia is a severe brain disorder involving significant breaks from reality, disorganized thinking, and problems with attention and memory. It is distinct from dissociative identity disorder (DID). Symptoms are categorized as negative (e.g., social withdrawal, catatonia) and positive (e.g., hallucinations, delusions). The disorder progresses through prodromal, active, and residual phases, with subtypes such as paranoid, disorganized, and catatonic schizophrenia.
Negative Symptoms: Social withdrawal, lack of motivation, catatonia.
Positive Symptoms: Hallucinations (e.g., hearing voices), delusions (paranoid or grandiose beliefs), disorganized behavior.
Phases: Prodromal (onset of negative symptoms), active (positive symptoms), residual (reduction in symptoms).

Example: A teen may report hearing their mother's voice when she is not present, illustrating auditory hallucinations.

Explanations and Causes
Schizophrenia has multifactorial causes, including genetic, neurobiological, and environmental factors.
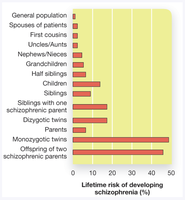
Genetics: Family and twin studies show a strong genetic component. The risk increases with genetic relatedness to an affected individual.
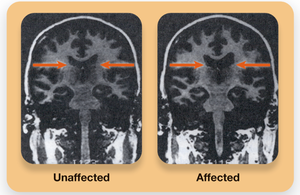
Brain Differences: Enlarged ventricles, reduced frontal cortex activity, increased dopamine (DA) activity (positive symptoms), and underactive glutamate (GLU) systems (negative symptoms).
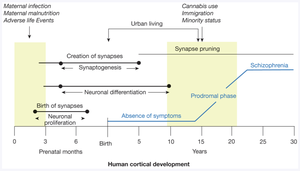
Neurodevelopmental Hypothesis: Prenatal factors (e.g., maternal stress, malnutrition) and adolescent factors (e.g., excessive synaptic pruning in the prefrontal cortex) contribute to risk.
Environmental Stressors: Urban living, low social support, high emotional expressiveness (EE), and cannabis use increase risk.
Additional info: Early intervention and social support can improve outcomes for individuals with schizophrenia. Treatment often involves antipsychotic medications and psychosocial interventions.
