Back
BackSocial Determinants of Health: Concepts, Frameworks, and Policy Implications
Study Guide - Smart Notes

Introduction to Social Determinants of Health
Overview
The social determinants of health (SDH) are the social, economic, and political factors that influence the health of individuals and populations. Understanding SDH is essential for addressing health disparities and promoting health equity within societies. This topic is foundational in sociology, public health, and health policy studies.
Differing Concepts of Health
Definitions and Approaches
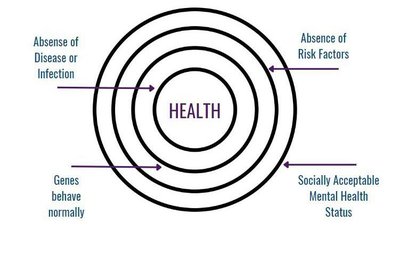
Medical (Traditional/Biomedical) Approach: Health is defined as the absence of disease or disability. Focuses on physiological risk factors and disease categories such as cardiovascular disease, diabetes, and mental illness.
Behavioural (Lifestyle) Approach: Health is seen as a result of individual choices and behaviors, such as diet, exercise, and substance use. Emphasizes health education and lifestyle modification.
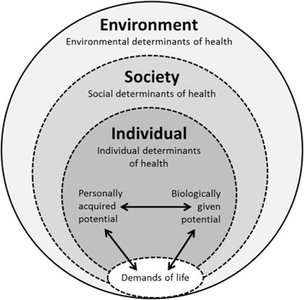
Socio-Environmental (Societal) Approach: Health is a positive state influenced by social connections, community support, and environmental conditions. Focuses on psychosocial risk factors like poverty, social isolation, and hazardous environments.
Political Economy (Structural-Critical) Approach: Health is linked to the equitable distribution of resources and power within society. Examines how institutions and class structures affect health outcomes.
Each approach leads to different definitions of health problems, strategies for solutions, target groups, and responsible actors.
Medical (Traditional/Biomedical) Approach
Principal Strategies: Surgical interventions, drug therapies, health care, screening for risk factors.
Target: High-risk individuals.
Actors: Physicians, nurses, allied health workers.

Behavioural (Lifestyle) Approach
Principal Strategies: Health education, social marketing, advocacy for supportive public policies (e.g., smoking bans).
Target: High-risk groups, children, and youth.
Actors: Public health workers, advocacy groups, governments.



Socio-Environmental (Societal) Approach
Principal Strategies: Community development, coalition building, political action, societal change.
Target: High-risk societal conditions.
Actors: Citizens, social development organizations, political movements.
Political Economy (Structural-Critical) Approach
Principal Strategies: Political action by organized labor, regulation of business, health-supporting public policies.
Target: Influence of the wealthy and powerful.
Actors: Political movements and parties.
Social Determinants of Health (SDH)
Definition and Importance
SDH are the economic and social conditions that shape the health of individuals, communities, and entire jurisdictions. They determine the quantity and quality of resources available to members of society, influencing health outcomes and disparities.
Examples of SDH: Income, education, employment, housing, food security, social exclusion, access to health services, and more.
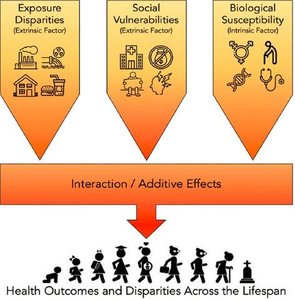
Impact: SDH can lead to inequities in exposure to unhealthy environments, affect individual behaviors, increase vulnerability, and limit access to services.
Frameworks for Understanding SDH
Canadian SDH Focus: Indigenous ancestry, disability status, early life, education, employment, food security, health services, gender, housing, income, racism, social exclusion, social safety net, unemployment.
Health Equity and Inequity
Definitions
Health Equity: The absence of unfair, avoidable, or remediable differences among groups of people. Achieved when everyone can attain their full health potential.
Health Inequity: Systematic, avoidable, and unfair differences in health associated with social disadvantage. These are modifiable and relate to differences in opportunity.
Health Inequality: Measurable differences in health between individuals, groups, or communities, which may be natural or unavoidable (e.g., genetics, age).
Public Policy and Health
Shifting the Focus
Health care spending alone cannot reduce health disparities.
Poverty and social disadvantage are primary drivers of poor health outcomes.
Governments must focus on health promotion, prevention, and addressing root causes such as income, housing, and education.
Healthy lifestyles are insufficient without social supports.


Geographical Patterns of Health and Social Determinants in Toronto
Spatial Distribution of Health and Social Factors
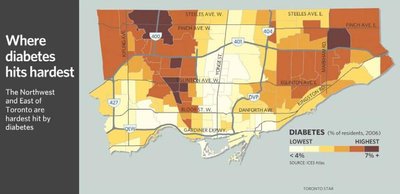
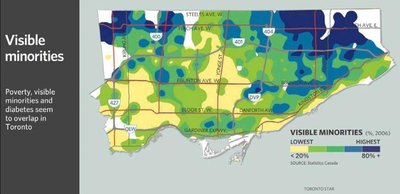
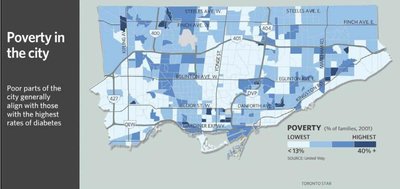
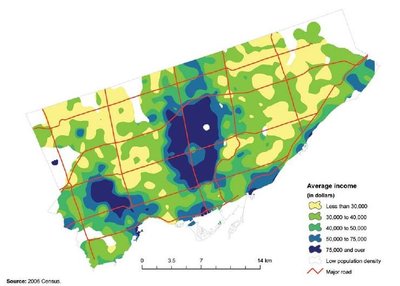
Maps of Toronto neighborhoods reveal that diabetes, poverty, and visible minority populations often overlap geographically, indicating the influence of SDH on health outcomes.
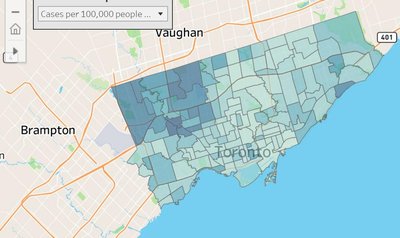
Crime rates, income, and other social indicators also show spatial patterns that align with health disparities.
Map | Variable | Key Insight |
|---|---|---|
| Diabetes | Higher rates in Northwest and East Toronto |
| Visible Minorities | Higher concentrations overlap with high diabetes areas |
| Poverty | Poorer areas align with higher diabetes rates |
| Crime | Crime rates vary by neighborhood, often higher in disadvantaged areas |
| Income | Lower average income in areas with higher health risks |
Origins of Disease and Lifecourse Perspective
Accumulation of Risk
Health outcomes in adulthood reflect the cumulative influence of socio-economic circumstances throughout life.
Adverse conditions in early life can increase the risk of chronic diseases later in life.
Traditional vs. Social Determinants Approaches to Health Promotion
Traditional Ten Tips for Better Health
Focus on individual behaviors: not smoking, balanced diet, physical activity, stress management, moderate alcohol use, sun protection, safer sex, cancer screening, road safety, first aid knowledge.
Social Determinants Ten Tips for Better Health
Highlight the importance of social and economic conditions: avoiding poverty, having stable employment, living in quality housing, accessing benefits, and avoiding environmental hazards.
APA 7th Edition: Best Practices for Students
Academic Integrity and Citation
Use in-text citations for all ideas, data, or words from others.
Paraphrase instead of quoting directly.
Include a reference list with all cited sources.
Follow formatting rules: 12 pt. Times New Roman, double-spaced, 1-inch margins, page numbers, and title page.
Avoid plagiarism by properly crediting all sources.
Assignments and Course Requirements
Summary
Weekly chapter summaries, midterm paper, final paper, and final exam.
Strict deadlines and self-declaration policy for extensions.
Emphasis on academic honesty and critical engagement with material.
Conclusion
Understanding the social determinants of health is crucial for addressing health disparities and promoting equity. Sociological perspectives provide frameworks for analyzing how social, economic, and political factors shape health outcomes, guiding effective public policy and health promotion strategies.